
Dr. Amanda Berberich
Assistant Professor, Western University, and Endocrinologist, Division of Endocrinology & Metabolism, St. Joseph’s Health Care
We all produce and need cholesterol. But high amounts of the wrong kind can put us at risk of cardiovascular disease.
Cholesterol is a fat that’s found in our blood. Our bodies make it naturally, but it can also be increased through our diet. Cholesterol comes in two forms: low-density lipoprotein (LDL-C) and high-density lipoprotein (HDL-c). LDL-C is often referred to as “bad cholesterol” and for valid reason. “LDL particles carry high concentrations of cholesterol that can enter the blood vessel walls and cause plaque buildup. Over time this can cause narrowing of the arteries, which increases the risk for heart attack and stroke,” says Dr. Amanda Berberich, Assistant Professor, Western University, and Endocrinologist, Division of Endocrinology & Metabolism, St. Joseph’s Health Care in London, Ontario. HDL-c, on the other hand, is often referred to as “good cholesterol” because it works to remove excess cholesterol from your body
Cholesterol is measured through a blood test. A LDL-C reading below 3.0 mmol/l for children, adolescents and adults is considered ideal, while anything above 4.0 is considered high.
Genetically inherited high LDL-C conditions
Numerous factors can contribute to high cholesterol, such as nutrition, physical activity levels, and other medical conditions. However, some people have an inherited genetic condition known as familial hypercholesterolemia (FH) which makes them unable to remove the LDL particles from their bloodstream. “As a result, they can have more than double the normal amounts of LDL-C, which puts them at risk for early heart attack and stroke,” says Dr. Berberich. There are two types of FH—heterozygous hypercholesterolemia (HeFH) where the patient has one defective gene (HeFH affects about one in 250 Canadians1)and homozygous familial hypercholesterolemia (HoFH) where the patient has two defective genes (this is rarer and affects about one in 300,000 Canadians, although French Canadians have a higher prevalence).
Complicating matters is that patients with FH may be undiagnosed until they’ve had their first cholesterol screening at age 40. “By this point significant disease has often already developed and the window to intervene early to prevent disease onset has lapsed,” says Dr. Berberich. “Even when a level is checked, not all providers are aware of this potential diagnosis and the dangers it poses, and levels may be left unaddressed,” she says.
Few visible symptoms of LDL-C
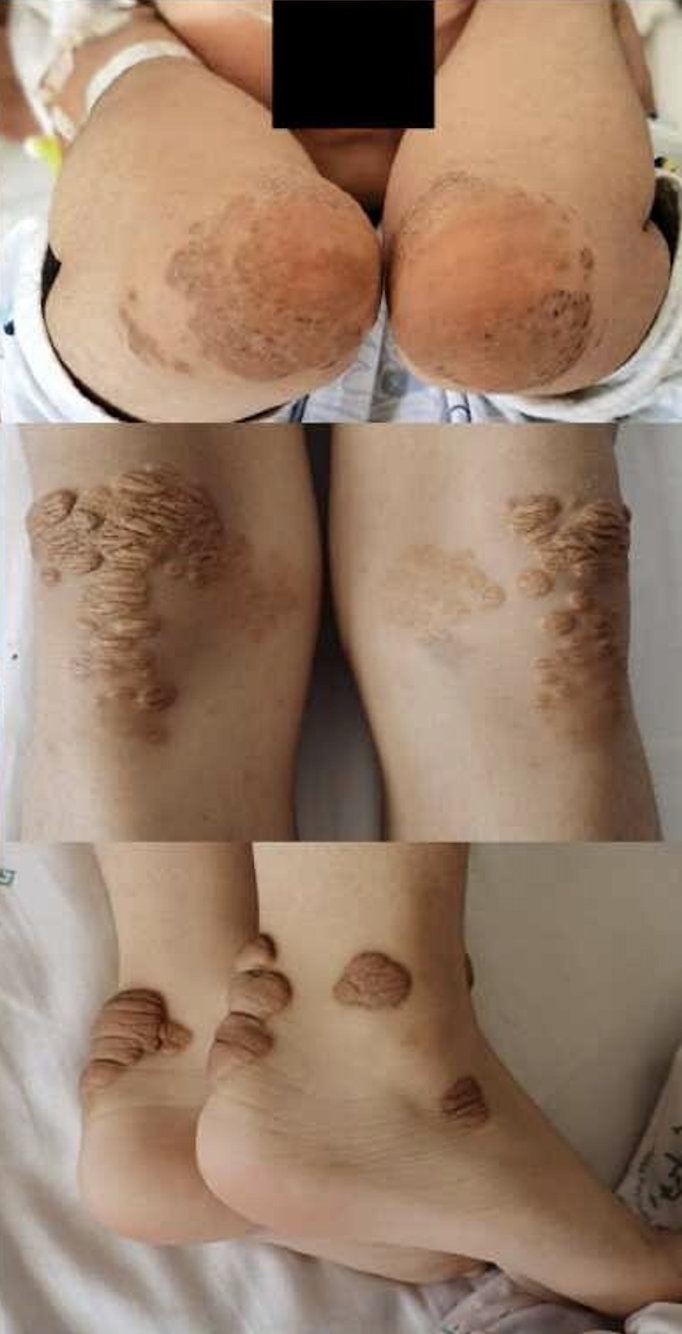
One of the challenges of high LDL-C is that it presents with few signs or symptoms. However, one physical manifestation is yellowish, fatty deposits on the tendons of the hand, Achilles tendon, other exterior tendons (tendon xanthomas) or in the corners of the eyes (xanthelasmas). “These often appear as yellowish, irregular bumps within or on the surface of the tendon,” says Dr. Berberich. “A yellow-whitish crescent in the lower portion of the cornea in an individual under age 45 can also be a sign,” she says.
For many individuals, however, there are often no signs of high cholesterol until it causes a heart attack or stroke. This may even be preceded by many years of silent, asymptomatic accumulation of plaque on the artery walls. “As plaque volume accumulates to a critical level, some patients start to develop chest tightness or shortness of breath when they become more active or experience cramping in the leg or back of the calf,” she says.
High LDL-C can indicate other, treatable conditions
While high LDL-C levels can be a sign of other treatable medical conditions such as hypothyroidism and diabetes, they most commonly signal a risk for cardiovascular conditions. The only way to get an accurate diagnosis is by having your cholesterol levels checked through a blood test.
An early and accurate diagnosis is critical to allow for early intervention and improved lifelong outcomes. “Risk is directly proportional to the amount of exposure to high cholesterol, so the higher an individual’s cholesterol and the longer they’re exposed, the greater the risk for disease development,” says Dr. Berberich. “Once cardiovascular disease develops, it’s much harder to reverse or even stabilize the process. Conversely, if treatment begins early and levels are well controlled, the risk is minimized,” she says.
What to do if you have high LDL-C
It’s important for everyone, including children, to get their LDL-C levels checked once. If you have high LDL-C, you want to address it immediately. Standard treatment typically involves lifestyle changes and medication. Eating a healthy diet, exercising, not smoking, maintaining a normal weight, and stress management are a good place to start but may not be sufficient on their own.2 “Most individuals will be started on a statin medication, which decreases cholesterol production in the liver,” says Dr. Berberich. “Other options, such as cholesterol inhibitors or PCSK9 inhibitors, which improve the clearance of cholesterol from the blood, may also be required if cholesterol levels start very high. For some of the rare genetic syndromes like HeFH and HoFH, we have targeted management strategies,” she says.
Before any treatment can begin, you need to know your LDL-C levels. “For individuals who may have FH, this is especially important as many are undiagnosed,” says Dr. Berberich. Because children with HoFH are at higher risk of early coronary events and death from heart attack than adults, early diagnosis and treatment are crucial to ensuring long-term survival.3
To learn more about FH, please visit: www.fhcanada.net and www.hofhdisease.ca.
This article was made possible with support from Ultragenyx.
- FH Canada
- Heart & Stroke
- Wang N, Wei Y, Zhou G, Zhang Y, Song J. Acute coronary syndrome in an 8-year-old child with familial hypercholesterolemia: a case report. J Med Case Rep. 2022 Jul 26;16(1):290. doi: 10.1186/s13256-022-03488-3. PMID: 35879787; PMCID: PMC9316422.


