Dr. Paul Wheatley-Price
Medical Oncologist, The Ottawa Hospital Cancer Centre & Associate Professor, Department of Medicine, University of Ottawa
Lung cancer has had a significant impact on Canadians, but patients now have more reasons for optimism with new treatments and screening programs.
Lung cancer is the most commonly diagnosed cancer in Canada and is also the leading cause of death from cancer for both men and women.1 It’s a disease that typically doesn’t have good outcomes, with 75 percent of cases diagnosed at stage 3 or 4. Diagnosing it earlier, before it has spread, may improve the chances of survival.
For well over a decade, Dr. Paul Wheatley-Price, a medical oncologist with The Ottawa Hospital Cancer Centre and an associate professor in the Department of Medicine at the University of Ottawa, has spent most of his practice focused on lung cancer. Increasing awareness, screening programs, and new treatment options are giving hope to those with the disease.
A new focus on screening and early diagnosis
Lung cancer screening programs will play an increasingly important role as progress continues to expand access. “Screening is quite new,” says Dr. Wheatley-Price. “What this does is take people at risk of lung cancer and offer them an annual CT scan of their chest, which can be done with very low exposure to radiation. Across the globe, we’ve known for several years that it will identify lung cancer successfully at stage 1 or 2 effectively. However, it’s quite new to Canada.”
Current guidelines recommend that high-risk adults ages 55 to 74, who currently smoke or have quit less than 15 years ago with a significant history of cigarette smoking, should be screened for lung cancer. Currently, screening is available sporadically across Canada — a key issue being addressed by Lung Cancer Canada (LCC). Dr. Wheatley-Price, who served as the organization’s president from 2016 to 2021, says that LCC is encouraging provincial health ministries to establish lung cancer screening programs and widen their availability.
“When I first got involved, there was no real patient advocacy,” he says. “Lung cancer is more common in older populations, rural populations, lower socioeconomic groups, and those with lower levels of education. And frankly, people weren’t surviving lung cancer. They didn’t have anyone advocating for them. Fortunately, through various initiatives, it’s much better now.”
Historically, we haven’t had very many good treatments. Now, that’s starting to change. As a result, we’re seeing survival rates improve.
New innovations help improve survival rates

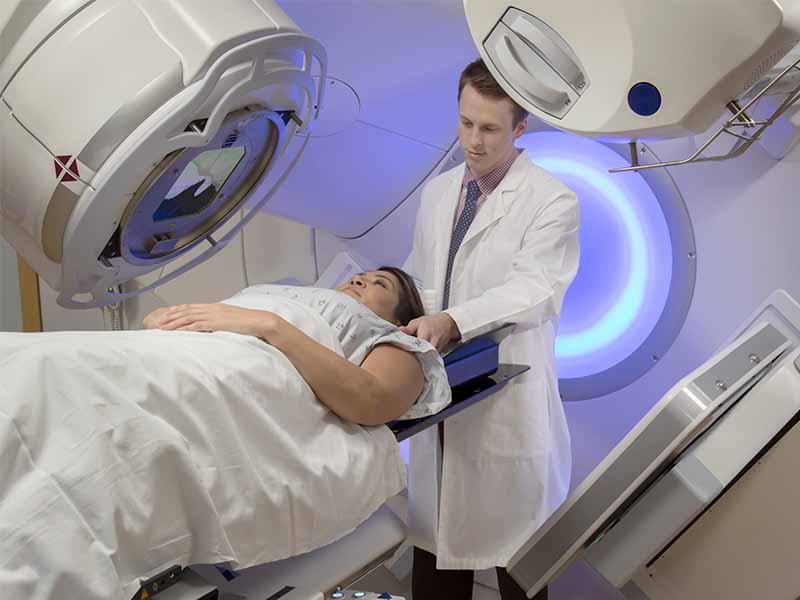
Physicians have several tools available to treat lung cancer, including surgery, radiation therapy, and chemotherapy. These may be used on their own or in combination. In recent years, targeted therapy* and immunotherapy** have been added as options, thanks to innovations in cancer research. “Historically, we haven’t had very many good treatments,” says Dr. Wheatley-Price. “Now, that’s starting to change. As a result, we’re seeing survival rates improve.” A decade ago, the chances a lung cancer patient would survive five years beyond their diagnosis was 13 percent. Based on the most recent data from 2021, the rate has increased to 22 percent. It jumped three percent over 2020, which is “the biggest improvement seen to date,” he notes.
“And it’s not because of screening,” Dr. Wheatley-Price adds. “It hasn’t been around long enough to impact the data. It’s because there are now more treatments helping people live a lot longer than they used to. And we hope that will continue to improve in the coming years. We’ve seen so many people with stage 4 lung cancer who are now multi-year survivors. Pre-immunotherapy, they wouldn’t have survived for as long. Now, immunotherapy is also effective in stage 3 lung cancer and is boosting the cure rates. It’s truly revolutionary and has completely changed the outcomes and health of many patients.”
It also takes a dedicated multidisciplinary health care team to create healthier futures — from physicians, like medical or radiation oncologists, respirologists, thoracic surgeons, pathologists, palliative care physicians, and radiologists, to nurses and allied health professionals such as occupational therapists, physiotherapists, social workers, personal support workers, and clerical staff. “Now, as a team, we’re able to offer people, if not a cure, at least realistic hope of living for much longer and much better than they may have imagined,” says Dr. Wheatley-Price. These efforts, coupled with new therapies, help patients achieve better outcomes.
This page was sponsored by one of Canada’s leading research-based pharmaceutical companies.
References
1 cancer.ca/en/cancer-information/cancer-types/lung/statistics
2 lungcancercanada.ca/Lung-Cancer/Living-with-lung-cancer/Talking-about-cancer.aspx
Definitions
*Targeted therapy: Some people with non-small cell lung cancer have targeted therapy. It uses drugs to target specific molecules (such as proteins) on cancer cells or inside them. These molecules help send signals that tell cells to grow or divide. By targeting these molecules, the drugs stop the growth and spread of cancer cells and limit harm to normal cells.
** Immunotherapy: Our immune system has the ability to find and destroy cancer cells. But cancer cells can sometimes hide from the immune system and avoid being destroyed. Cancer cells may also stop the immune system from working properly. Immunotherapy helps to strengthen or restore the immune system’s ability to fight cancer.
*** Non-small cell lung cancer: Non-small cell lung cancer usually starts in glandular cells on the outer part of the lung. This type of cancer is called adenocarcinoma. Non-small cell lung cancer can also start in flat, thin cells called squamous cells. These cells line the bronchi, which are the large airways that branch off from the windpipe (trachea) into the lungs. This type of cancer is called squamous cell carcinoma of the lung. Large cell carcinoma is another type of non-small cell lung cancer, but it is less common. There are also several rare types of non-small cell lung cancer. These include sarcoma and sarcomatoid carcinoma.