Mary Zawadzki
Manager of Community Programs & Resources, Melanoma Canada
In recent years, innovations to help the body’s immune system destroy cancer cells have been life-changing for patients.
Melanoma is more than skin deep. It’s a very serious form of skin cancer. In 2021, an estimated 8,700 Canadians learned that they had the disease — an increase of 8.5 per cent over the previous year. More than 1,200 died from melanoma in 2020. It can spread to other areas of the body, making it potentially deadly for anyone regardless of age, gender, or race.
Non-melanoma skin cancers are more common, with over 80,000 cases diagnosed each year. Basal cell carcinoma is the most commonly diagnosed, but it’s less deadly as it’s less likely to metastasize. Melanoma and non-melanoma cancers can have significant health consequences, underscoring the need for prevention (practising sun-safe behaviours, such as wearing broad-spectrum sunscreen), early detection, and effective treatment options. The leading cause for both types of cancers is ultraviolet exposure from the sun or artificial sources, such as tanning beds.
For patients whose cancer has metastasized or who didn’t benefit from radiation or surgery, there are other treatments, including immunotherapy.
Make early detection a priority
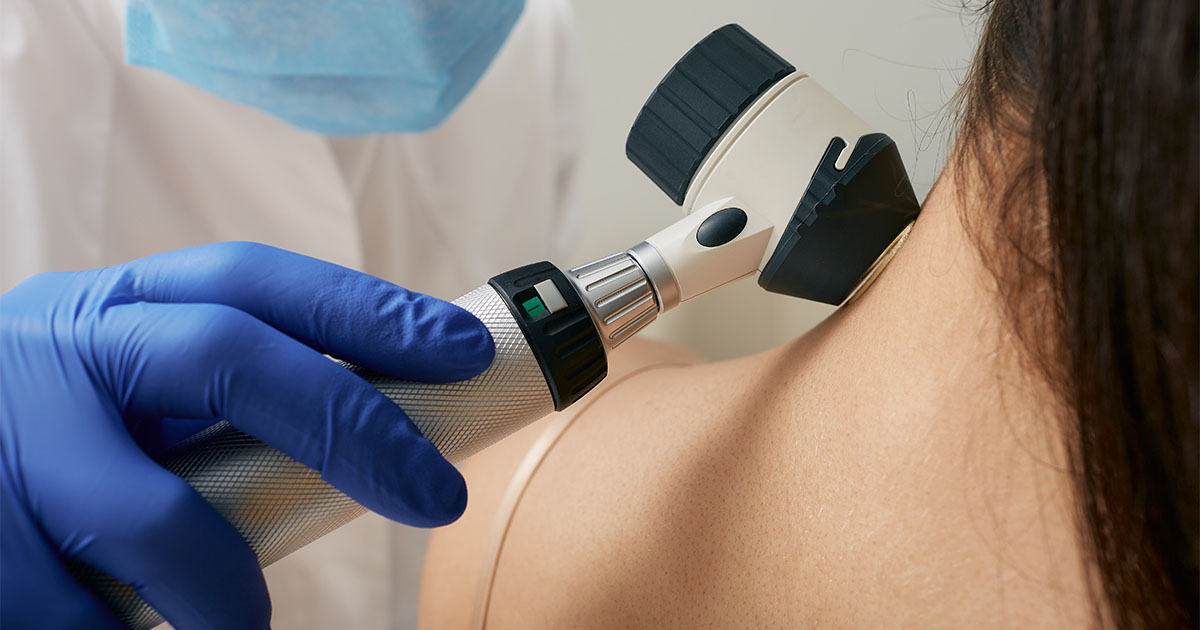
Compared to other types of cancer, signs of skin cancer are visible on a patient’s skin. With that in mind, experts suggest checking your skin and moles monthly. Look for asymmetry, irregular borders, colour, diameter (greater than six millimetres), and evolution (recent changes in moles). Should you spot anything troubling, talk to your doctor about getting a referral to a dermatologist, who may perform a biopsy of the suspicious skin lesion(s). If skin cancer is found, it can often be addressed through surgery or radiation, according to Mary Zawadzki, Manager of Community Programs and Resources at Melanoma Network of Canada.
“For patients whose cancer has metastasized or who didn’t benefit from radiation or surgery, there are other treatments, including immunotherapy,” says Zawadzki. “It’s one of the newer tools available, along with topical chemotherapy (a cream or gel applied directly to the skin, for example) and targeted therapy.” Immunotherapy uses drugs given intravenously to enable the body’s own immune system to destroy cancer cells. Meanwhile, targeted therapy is administered in pill form and focuses on tackling the specific gene mutations of a cancerous tumour.
Advanced tools for metastasized disease
Being diagnosed with melanoma just a decade ago was devastating to patients, Zawadzki notes. “If the disease couldn’t be controlled through surgery or radiation, an oncologist’s toolbox of treatment options was very limited. These new immunotherapies have been ground-breaking. They’ve allowed people to have a greater sense of hope that they can combat this disease. People can move forward and have a great quality of life.”
New treatments for cancer that has spread can also be used for melanoma and non-melanoma types, which include basal cell carcinoma (BCC) and cutaneous squamous cell carcinoma (cSCC). It’s rare that non-melanomas will spread, but it’s much more common with cSCC if left untreated. For early-stage localized cSCC, a doctor may remove it surgically or through freezing or scraping. These measures may not work if the cSCC is able to grow. For example, an cSCC on the cheek could metastasize to lymph nodes in the neck area. In cases of advanced disease, immunotherapy may be recommended.
As is the case with many cancer types, early detection is key, Zawadzki emphasizes. She suggests Canadians remain diligent about checking for changes in their moles and seeking medical attention without delay if any problems are identified.
This article was made possible with support from a leading research-based pharmaceutical company.