Stigmas toward people living with substance use disorders are one of the major barriers preventing people from accessing the care they need.
When it comes to people living with a substance use disorder, stigma has a profound impact on health. The labels we use — alcoholic, addict, user, or abuser — and the images of people on the street, marginalized, and facing poverty, serve only to set people living with a serious and chronic medical condition apart. There’s “them” and then there’s “us.” This is stigma.
The fact is, the vast majority of people living in Canada who use substances are us. We have a home, we have a job, and we live among family, friends, and our community. Statistics show that 78 percent of people in Canada over the age of 15 use some form of psychoactive substance and women in their late 30s and 40s, are among the fastest-growing demographic in Canada experiencing fatty liver disease, which is sometimes associated with high levels of alcohol consumption. You can probably picture someone you know right now.
Stigma is best understood as a deeply-held set of false beliefs about a group of people with at least one attribute in common. These beliefs allow for judgment, oppression, and discrimination through overt actions or silent complicity.
Stigma not only prevents people from receiving care for their substance use, it also prevents them from even seeking care in the first place. It stems from the belief that people who use substances are choosing to have a disorder. The science shows us, however, that the causes are a much more complex mix of adverse childhood experiences, trauma, genetics, and brain chemistry, among other factors.
The language we use has a direct impact on the quality of care. The image below illustrates the results of a study by John Kelly of Harvard University. Participants in the study were divided into two groups and asked to read aloud a narrative about substance use. Both narratives were identical, except in one, the term “substance abuser” was used, and in the other, “substance use disorder.”
As shown in the graph below, the difference in responses attributing blame, believing that punishment is deserved, or believing that treatment should be offered is significant. More striking, even when using a medically-appropriate term — “substance use disorder” — 23 percent of respondents still believed that people with a medical condition should be punished, 42 percent saw them as a social threat, and 31 percent thought that they’re undeserving of treatment.
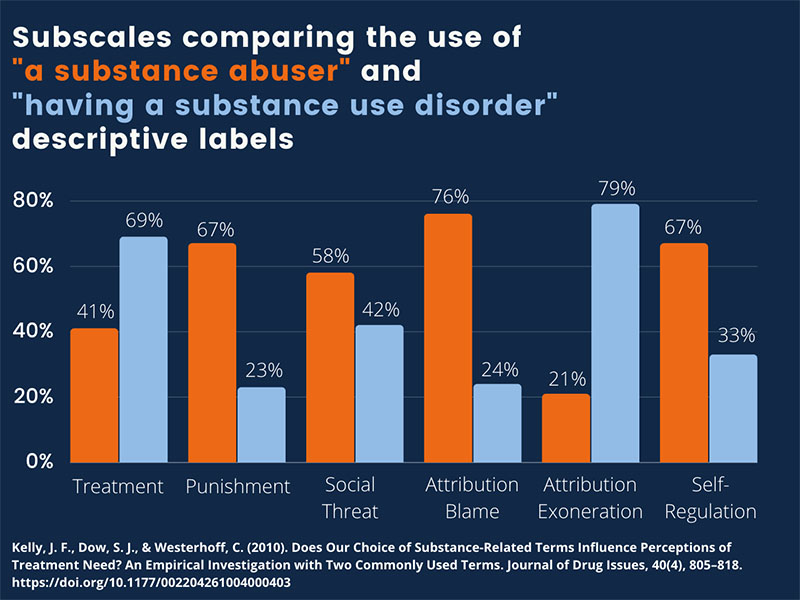
Perhaps most alarmingly, the subjects of the study were members of medical professions — a clear indication of how embedded stigma is in our health systems. The research shows that people with substance use disorders are the most stigmatized population in the health field. Reframing our language is not just a “nice to have” or an exercise in political correctness — it’s a life-saving necessity.
What can we do? Education is key, and better yet, education provided by organizations like CAPSA, which employs subject matter experts with lived and living experience. Direct contact with those who experience stigma is shown to be the best practice for reducing stigmas and twice as effective as education alone. Allies need to see, hear, and feel the impacts of stigma, challenge their biases, and correct misunderstandings at the source, in teachable moments and in a non-threatening environment. Although there’s plenty of evidence that links a reduction in stigma to a gross reduction in health costs (physical and financial), challenging stigma isn’t an intellectual exercise. It must be felt and experienced to be understood.
Education, combined with using medically-appropriate terms (instead of pejorative labels) and person-first language, is the first step toward dismantling stigma and improving health outcomes. I’m Anthony, a person with a substance use disorder. I’m not a disordered person in general, nor would I want to be defined by my condition first or solely. Would you?
The cost of substance use in Canada is staggering. In 2017, $46 billion was spent on health care, lost productivity, and criminal justice. Nearly 63 percent of these costs were related to the consumption of alcohol and tobacco. With the impact of COVID-19 on substance consumption, these costs are anticipated to rise.
But the personal costs are even higher. For every person living with a substance use disorder, five family members, friends, and co-workers are affected by someone they care about. The issue impacts millions of people living in Canada. It’s time to end the suffering and respect all those whose health needs care.

Anthony Esposti
Chief Executive Officer, CAPSA
A little bit about me
I currently live well with both mental health concerns and a substance use disorder. My path to lead CAPSA was blocked by the internalized and societal stigma I faced surrounding my diagnosis. It kept me from publicly discussing issues around my substance use health, not only when I was most in need of health care but even after I got well. While images and stories we see often depict substance use disorder as a desperate issue of poverty, housing insecurity, and social separation, I lived comfortably indoors, had meaningful work, and was surrounded by family and friends — similar to 85 percent of those like me. Yet, due to stigma, I couldn’t ask for help and I couldn’t let people know that I got well. I’ll let you decide what desperation looks like.



